
3D printed surgical instruments are changing the medical industry through groundbreaking design capabilities and affordable production. Traditional instrument trays made from stainless steel cost over $50,000 per tray. 3D printing offers a more economical option with better functionality. The global population aged 65 or older will reach about 20% by 2050, creating an urgent demand for innovative medical solutions.
3D printed surgical instruments offer remarkable customization options through their design and fabrication process. Companies like restor3d now use fleets of over 25 Formlabs 3D printers in their production lines, showing how the industry has embraced this technology. Quick design iterations based on surgeons’ feedback lead to more effective tools. This technology creates surgical instruments with intricate features, internal channels, and ergonomic forms that were impossible or too expensive to manufacture before.
The technology also makes precise fabrication of complex metal implants possible based on injured tissue anatomy. Objects built layer by layer can take virtually any shape, which allows multiple components to combine into a single part. These tools become lighter, easier to assemble, and often cost less to produce. This revolutionary force tailors instruments not just to procedures but potentially to individual patient anatomy or surgeon priorities, marking an important change toward tailored surgical care.
Challenges with Traditional Surgical Tools and Implants
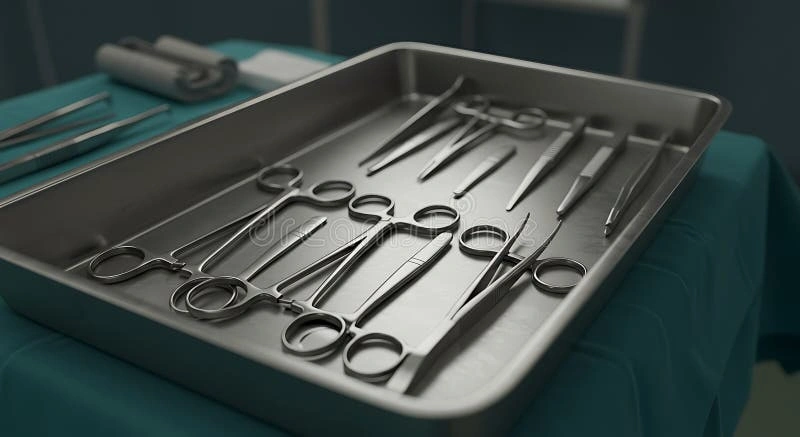
Traditional surgical tools and implants face many challenges that don’t work well in modern healthcare settings. These shortcomings have led researchers to explore other options like 3D printed titanium instruments and patient-specific implants.
High Cost of Stainless Steel Instrument Trays
Healthcare facilities struggle with the financial load of traditional stainless steel instrument trays. Simple stainless steel surgical trays might cost as little as EUR 7.36. Yet complete instrument sets for specific procedures need substantial investment. A study of preference cards for laparoscopic cholecystectomy procedures showed disposable supply costs varied from USD 92.00 to USD 637.00, with average costs hitting USD 333.00.
The financial strain goes beyond the original purchase costs. Operating rooms generate both major revenue and waste among hospital departments. Surgical instrument errors heavily affect operating room efficiency. These mistakes lead to yearly lost charges between USD 6,751,058.06 and USD 9,421,590.11. Each affected case loses an average of 10.16 minutes of valuable operating room time.
Lack of Customization in Conventional Implants
Mass-produced conventional implants available to more people today have clear limitations. These devices come in set shapes and sizes that don’t deal very well with each patient’s unique needs. This one-size-fits-most approach becomes a real problem, especially when you have special cases.
Dental applications show the drawbacks of standard implants clearly. Problems include surgical invasiveness from bone drilling needs and possible crestal bone loss around the implant. The mismatch between standard implants and a patient’s anatomy creates issues that influence both function and long-term results.
These customization limits reach beyond dental work into orthopedic, craniofacial, and other implant types. Traditional manufacturing methods restrict knowing how to create truly patient-specific solutions matching individual anatomical features. Poor fit often results from this lack of customization, which can hurt functional outcomes and patient satisfaction.
Sterilization and Inventory Burdens in Hospitals
Healthcare facilities face a critical challenge with traditional surgical instrument sterilization. Research reveals concerning failure rates in sterilization processes. Vaporized hydrogen peroxide (VHP) failed to sterilize surgical tools completely 76.3% of the time when tools had salt or blood contamination without proper cleaning beforehand. Other methods like HPGP and ETO showed failure rates of 1.9%, which shows how complex it is to ensure sterile instruments.
Inventory management creates another major burden. Operating room environments often waste resources and run inefficiently. Most hospitals lack a standard process to manage materials. Traditional instruments get grouped into containers called trays. Opening a tray means all items need complete sterile processing, whether used or not. This wastes labor and sterilization resources on untouched instruments.
Preference cards – lists of surgeon-required items – add to these inventory challenges. Surgeons often request materials just to be safe rather than based on actual patient needs. This forces healthcare facilities to stock excess quantities, creating storage problems and financial pressure. Most hospitals can’t track perpetual inventory for operating suites, which makes manual tracking almost impossible in busy clinical settings.
Analysis shows that 88.6% of surgical instrument errors link to problems with visualization needed to identify, check functionality, spot bioburden, and put instruments in correct trays. These issues highlight the need for new technology to address the basic limitations of traditional surgical tools and implants.
Titanium 3D Printing for Custom Implants

Titanium 3D printing is changing how we make medical implants. This new approach helps create implants that match each patient’s unique anatomy perfectly. Patients no longer need to adapt to standard implants because doctors can now make custom devices that fit them exactly.
Patient-Specific Design from CT/MRI Imaging
Making custom titanium implants starts with detailed medical imaging. Doctors get CT or MRI scans to capture all the anatomical details they need for implant design. Software like Simpleware turns these 2D medical images into 3D models. The software uses both manual work and AI to segment the images. This helps rebuild anatomical structures accurately and get precise measurements for the implant.
Engineers then take the 3D model into design software to customize it further. A team at Duke University created a system where they could upload patient CT scans into software that lets them work with 3D bone and joint models. Senior surgeons worked with engineers to design implants that matched specific patient needs.
The next step converts polygon models to stereolithography format to prepare for manufacturing. Surgeons can control every detail of the implant design, which helps them create devices that fit the patient’s anatomy perfectly.
Titanium’s Biocompatibility and Osseointegration
Titanium is the best material for implant biocompatibility. It does more than just work well with the body – it forms direct connections with bone tissue through osseointegration. Research shows that porous titanium structures help bone grow directly onto them without needing bone grafts.
Scientists compared titanium implants with rough, perforated surfaces to smooth ones. The results showed that the body accepted both types well, but the bone grew better on textured surfaces. After 15 weeks, textured implants had strong bone growth directly on their surface. However, 30% of smooth implants showed gaps between the bone and implant.
The pores in 3D-printed titanium structures play a key role in bone integration. Scientists can adjust the porosity and structure to match natural bone properties. Tests showed that properly designed porous samples had compressive elastic moduli between 1 and 3.5 GPa, which is similar to natural spongy bone. This creates perfect conditions for bone cells to grow and multiply.
Use of Ti-6Al-4V in Orthopedic and Spinal Implants
Ti-6Al-4V (Grade 5 titanium) is the most common titanium alloy in orthopedic implants. It comes in two types: standard Ti-6Al-4V and Ti-6Al-4V ELI (Extra Low Interstitial). Both contain 6% aluminum, 4% vanadium, and the rest is titanium.
Ti-6Al-4V ELI bends better and resists fractures more effectively, which makes it perfect for implants that need to handle movement and stress. A study found that ELI implants in the spine broke 25% less often than standard alloy implants. This makes it great for spine implants, children’s devices, and facial reconstruction where strength matters most.
Electron beam melting (EBM) works best for making these custom implants. This method uses an electron beam in a vacuum to melt layers of titanium powder. The final product meets ASTM F136 standards for medical implants.
These custom titanium implants make a real difference in patients’ lives. A study of 15 patients who got 3D-printed titanium implants between 2014 and 2016 showed success in 13 cases. Patients had much less pain and said they would choose the same procedure again to keep their foot or ankle working well.
Designing 3D Printed Surgical Instruments
Medical teams need a methodical design approach to create effective 3D printed surgical instruments that balance functionality, ergonomics, and specific surgical requirements. 3D printing has changed everything by opening new possibilities for instrument customization that weren’t possible before.
Procedure-Specific Tool Development
Surgeons recognize opportunities to improve existing instruments first. 3D printed tools serve specific surgical procedures, unlike traditional multi-purpose instruments. This streamlines processes and reduces complexity.
Computer-Aided Design (CAD) software like SolidWorks is the foundation of developing digital models for surgical instruments. Designers translate surgeon requirements into precise digital specifications. A documented case study showed researchers spent about 20 hours on design time, and each instrument needed 4 iterations to work. This customization helps create procedure-specific instruments at a much lower cost than traditional manufacturing methods.
This idea goes beyond basic instruments to specialized tools. Companies like restor3d lead the way in developing procedure-specific and patient-specific instrumentation. They’ve created an agile process that connects surgeon’s needs with product development. Their just-in-time manufacturing capabilities outperform traditional production methods.
Ergonomic and Lightweight Instrument Design
Ergonomics is a vital part of surgical instrument effectiveness. 3D printing lets designers create lightweight, ergonomically optimized instruments that help surgeons stay comfortable during long procedures. Traditional stainless steel instruments can tire surgeons during extended operations. 3D printed titanium instruments offer excellent strength-to-weight ratios and reduce hand strain.
Designers focus on better grips, optimal weight distribution, and improved tactile feedback. To cite an instance, see how researchers modified surgical forceps based on surgeon feedback. They added better gripping surfaces, wider resting positions, thicker arms, and rounded crotches to increase stiffness. These ergonomic improvements matter because surgeons use forceps to handle delicate tissues and find subtle tissue planes—tasks that need accurate tactile feedback and excellent ergonomics.
3D printed instruments’ lightweight nature offers several benefits:
- Surgeons experience less fatigue during long procedures
- Better control and maneuverability improve precision
- Less material use can lower production costs
Integration of Surgeon Feedback in Iteration
Surgeon feedback guides the iterative development process, which is the most valuable aspect of 3D printed instrument design. This shared approach cuts traditional development time from years to weeks or days.
Teams test designs through simulated surgery and cadaveric testing. Simulated surgery helps improve ergonomics as surgeons handle instruments in non-surgical settings. Cadaveric testing reveals how well instruments work during actual surgical procedures.
A great example comes from needle drivers used in inguinal hernia repairs. The original designs had problems when surgeons applied significant force to suture needles – the needle driver tips would cross and drop needles. Designers used surgeon feedback and SolidWorks analysis to create a better version. They embedded one arm into another, which distributed force equally along the hinge’s axis and stopped tips from crossing.
Successful manufacturers of 3D printed surgical instruments stay in constant touch with surgeons. One manufacturer says, “We get feedback from surgeons constantly. 3D printing allows us to quickly iterate on the design to take surgeons’ feedback and deliver a new solution quickly”. This quick development cycle has changed how surgical instruments evolve to meet clinical needs.
3D Printing Surgical Instruments: The Design and Fabrication Process
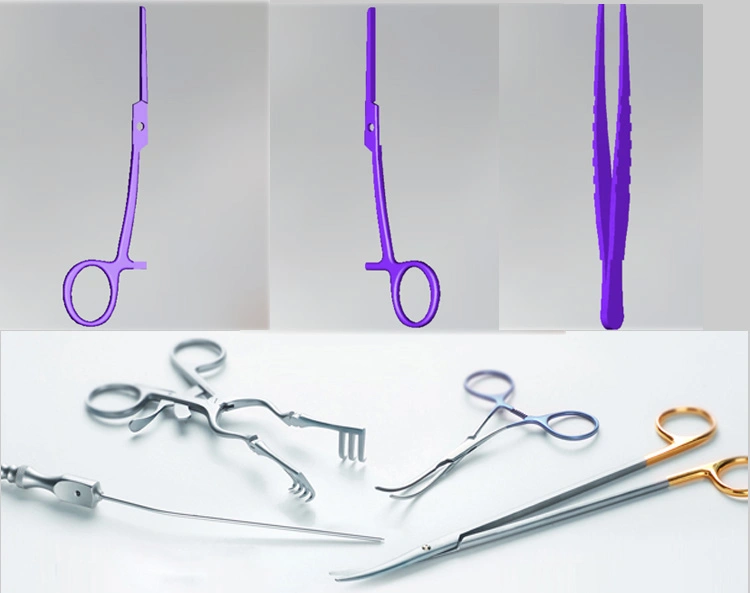
The path from concept to a physical 3D printed surgical instrument has multiple sophisticated technical stages. Each stage needs precise execution. This precision helps ensure the final titanium instrument meets surgical standards.
CAD Modeling and STL Conversion
Computer Aided Design (CAD) starts the manufacturing process by creating precise digital models of surgical instruments. Both open-source and proprietary CAD programs work well here. Autodesk Fusion 360 and SolidWorks are popular choices for medical device creation. A case study showed researchers using SolidWorks to design a complete surgical set. The set had hemostats, needle drivers, scalpel handles, retractors, and forceps. The design phase takes substantial time. Teams spend about 20 hours on total design time. Each instrument needs an average of 4 iterations to work properly.
The CAD model must transform into Standard Tessellation Language (STL) format once it meets specifications. STL shows the object as a mesh of triangles. This process “slices” the 3D model into layers for printing. The STL file has vital geometric data that helps the printer build the physical object layer by layer. Some complex anatomical data might need specialized software like Amira or 3D Slicer before conversion. The conversion process might limit the CAD model’s accuracy or precision.
Selective Laser Melting (SLM) for Titanium Tools
Selective Laser Melting (SLM) is the best technology to make titanium surgical instruments. This powder bed fusion process employs a precise laser beam that melts consecutive layers of titanium powder. Parts made through SLM are remarkably dense. Their density is a big deal as it means that they exceed 99.9% and have better mechanical properties than cast parts.
Machine-specific software takes the STL file and creates build instructions to start the SLM process. Different machines offer various build envelope sizes. The Sinterstation HiQ provides a W15 x D13 x H18 inches build space. Teams place instruments to minimize the build height for better efficiency. This placement reduces fabrication time. One example showed that a 3-inch build height took 6 hours to create a complete surgical set.
Commercially pure titanium Grade 2 is common for titanium instruments. Some applications just need titanium alloys like Ti-6Al-4V to get better mechanical properties. The SLM 250HL machine (SLM-Solutions) can process these materials with high precision.
Support Structure Optimization for Cleanability
Support structures are vital in the SLM fabrication process. They serve three key functions. They keep the unmolded powder layers stable during fabrication. Without good support, large suspending parts would collapse as powder falls. They help alleviate warping and deformation from rapid heating and cooling which creates large shrinkage stress in parts. They also connect the matrix and parts. This connection prevents losing dimensional accuracy that would happen if parts were molded directly on the matrix.
Different types of support structures exist with specific performance features. Dendritic supports look like branches with a 0.1 mm apex diameter and 0.6 mm base diameter. E-stage supports use a grid pattern. They have 0.1 mm top supports and 0.5 mm bottom supports. Conical supports are simple cone shapes similar in size to dendritic supports.
Stress distribution varies among these support types. Tests show E-stage supports have the smallest maximum displacement at 0.119 mm. Dendritic supports show 0.136 mm, and conical supports reach 0.241 mm. E-stage supports use more material volume (357.873 mm³) than dendritic supports (104.692 mm³) [2].
The build phase ends with post-processing. This step breaks parts out of the part cake and removes excess powder with a bead blaster. Post-processing helps the final instrument meet both functional and cleanability requirements for surgical use.
Post-Processing and Sterilization Readiness
3D printed titanium surgical instruments need significant post-processing steps to work properly and stay biocompatible in medical applications. These refinements will give you a sterile, patient-ready medical device from the raw printed part.
Stress Relief and Heat Treatment for Titanium
New titanium components have the most important residual stress you need to fix before clinical use. Heat treatment is a vital step that happens while parts stay attached to the build plate. You need temperatures between 600–800°C for 1-2 hours in vacuum furnaces or under argon-protective atmospheres. The aviation industry standard says vacuum working pressure should stay at least 2×10-3Pa to avoid vacuum surface corrosion.
Heat treatment environments require exact control because titanium reacts easily and can get contaminated by carbon, oxygen, and hydrogen. This contamination can harm the alloy’s properties. The chemical activity of titanium means you need very specific process settings, so when using argon as protection, gas purity must be above 99.99%.
Hot Isostatic Pressing (HIP) works well with heat treatment for critical applications. The process runs at 920–930°C under 100–120 MPa for 2–4 hours. This extra step removes internal porosity and boosts the mechanical properties you need for surgical instruments.
Surface Finishing: Electropolishing and Tumbling
Medical devices’ surface quality is vital since burrs and microcracks can trap contaminants and lead to corrosion. Electropolishing, also known as “reverse plating,” takes away a microscopically precise layer of surface material. This creates an ultra-smooth, defect-free finish.
This electrochemical process puts titanium instruments in a temperature-controlled chemical bath (usually 170-180°F) where they act as the positively-charged anode. Electric current flows through the electrolyte solution and dissolves metal ions from the surface. The process removes protrusions first through anodic leveling. The controlled metal removal:
- Gets rid of burrs and surface defects
- Boosts corrosion resistance
- Makes cleaning and sterilization better
- Cuts down pathogen adhesion
Tumbling offers another way to deburr and create a uniform surface texture. Both processes help the final instrument perform better and support safer surgical outcomes.
Sterilization Compatibility: Autoclave and Gamma
Medical applications require instruments that can handle repeated sterilization. Titanium instruments must keep their structure and surface properties intact through multiple cycles.
Autoclave sterilization uses high-pressure steam (121°C, 18 psi) for about 20 minutes. Titanium’s excellent thermal stability means 3D printed instruments handle these conditions without warping or breaking down—unlike many polymer alternatives.
Gamma irradiation works great as another option. It can sterilize pre-packaged materials with high-energy radiation that damages microorganism DNA without leaving toxic residues. The radiation penetrates deep into titanium instruments without raising the material temperature much.
Different sterilization methods change titanium’s surface properties in unique ways. Research shows these methods can affect surface hydrophobicity and change the outermost molecular layer’s chemical makeup. This might influence how the instrument interacts with the surrounding host tissue. Manufacturers must confirm that post-sterilization properties match the instrument’s intended use.
Healthcare facilities now use more 3D printed titanium instruments. Understanding these post-processing requirements will give you both regulatory compliance and the best clinical performance.
Clinical Impact and Surgeon Adoption
Medical surgeons choose titanium 3D printed instruments based on proven clinical benefits. These benefits directly affect surgical results, patient healing, and hospital efficiency.
Reduced OR Time with Patient-Matched Guides
Patient-matched 3D printed guides save valuable time in surgeries. A single printed guide cut full-arch restoration time in half – from 90 to 45 minutes. Surgeons can plan implant placement better, which speeds up procedures and reduces anesthesia time. They can also practice complex surgeries on 3D-printed models beforehand.
The benefits go beyond the operating room. Patient-specific implants and tools optimize the entire surgical process. Hospitals can treat more patients because procedures take less time.
Improved Accuracy in Implant Placement
3D printed surgical guides excel at precise implant placement. Research shows that guides without sleeves place implants more accurately. They reduce errors in crestal position, apical position, and angle. Guides without metal sleeves had much better angle accuracy (median = 1.442°) than those with metal sleeves (median = 3.883°).
Dentists use 3D printed guides made from CBCT scans and digital impressions. These guides control drilling depth, angle, and position exactly. The drill stays locked in the planned position, which leads to fewer problems and faster recovery.
Case Study: ACDF System with Printed Tools
3D printed titanium tools have transformed anterior cervical decompression and fusion (ACDF) procedures. A study of 157 patients using a new 3D-printed titanium interbody spacer with built-in screws showed average surgery times of 126.3 minutes.
The custom-fit ACDF cage system worked faster than standard tools. Surgeons removed less surrounding tissue while placing implants correctly.
These 3D-printed titanium spacers use porous supports to help bone grow where it meets the implant. Better design and simpler surgical methods led to higher survival rates compared to regular allograft spacers and anterior plating systems.
Scalability and Production Flexibility
Medical facilities can adjust their 3D printed surgical instrument production by managing printer fleets and on-demand manufacturing. This approach makes titanium printing a viable option for medical applications.
Fleet Management of SLA and Metal Printers
Setting up an additive manufacturing center helps build a resilient supply chain while cutting costs. Companies like Amnovis showcase successful fleet management results. They have produced more than 50,000 3D printed medical implants since 2021. The process has become simpler with affordable desktop and benchtop resin printers paired with compact SLS options. Companies typically run their production across multiple machines through automated fleet management systems. These systems work with internally developed ERP, MES, and APS platforms.
On-Demand Manufacturing for Low-Volume Needs
Medical device manufacturers can produce small quantities without compromising quality or speed through on-demand manufacturing. This method works best for medical devices that need 10,000 to 50,000 parts or fewer. Companies can eliminate extra warehouse space and financial risks by producing components as needed. 3D printing emerges as the most budget-friendly option for volumes under 200 parts.
Cost Efficiency Compared to Traditional Machining
Traditional manufacturing requires expensive tooling that costs over USD 50,000. In contrast, 3D printing uses low-cost aluminum tooling that reduces financial risk. This benefit stands out when production volumes cannot justify traditional tooling costs. Manufacturing costs decrease as production volumes go down.
Future of Titanium 3D Printing in Medicine
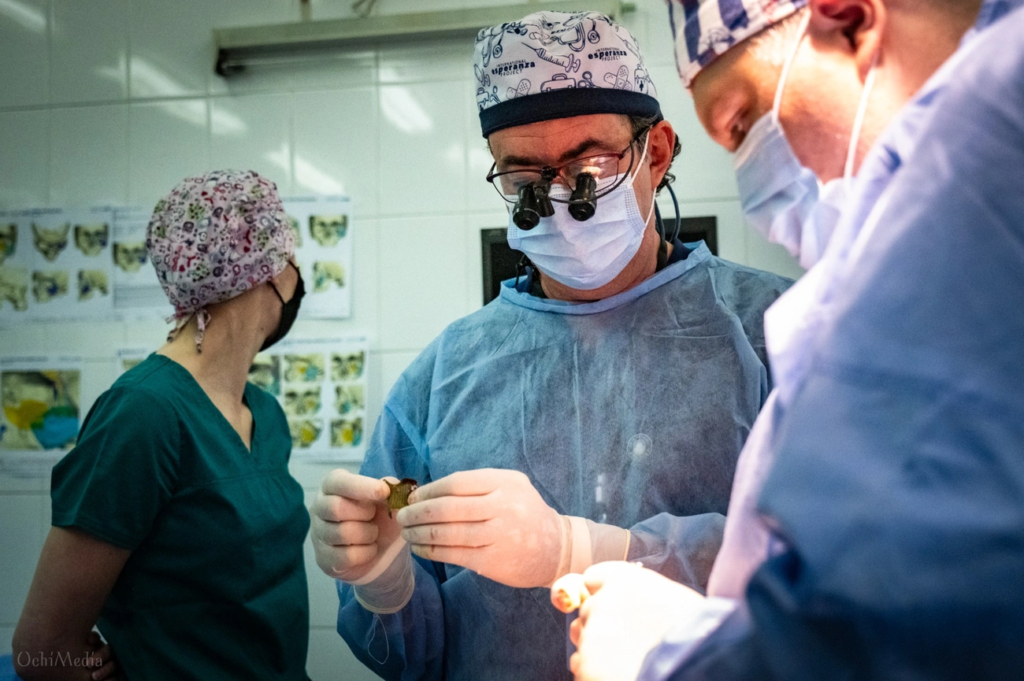
Titanium 3D printing technology goes beyond its current uses and creates new possibilities in medical treatment for specialties of all types. This state-of-the-art manufacturing method will revolutionize patient care through specialized applications that go together with other technologies.
Expansion into Foot, Ankle, and Oncology Applications
Medical specialists are adopting titanium 3D printing faster than ever. Musculoskeletal oncology teams now make customized implants for complex reconstructions with improved 3D printing technology. Recent clinical studies show good functional and cancer-related results in patients with malignant bone tumors in difficult areas like the sacrum and pelvis. Patient-specific implants (PSIs) match each person’s bone structure exactly, which helps doctors safely remove and rebuild damaged bone. Medical teams turn high-resolution CT scans into virtual 3D models that guide the manufacturing process.
Integration with AI and Surgical Planning Software
AI technology makes surgical planning better by finding vertebral features automatically. New software can spot healthy bone, measure tumor size, and create bone tumor removal plans in just 20–30 minutes. Doctors can test virtual bone cuts in different spots to find the best correction site. On top of that, AI helps plan surgeries by showing possible outcomes and finding the best implant positions. The combination of artificial intelligence with 3D printing makes surgical procedures like TLIF (Transforaminal Lumbar Interbody Fusion) more precise.
Regulatory Pathways for Custom Devices
Regulatory frameworks are changing to handle the unique challenges of custom 3D-printed medical devices. The FDA groups medical devices based on how much oversight they need for safety and effectiveness. Most FDA-cleared 3D-printed devices get approval through the 510(k) Premarket Notification pathway. Point-of-care (POC) manufacturing creates special regulatory challenges because it mixes the roles of healthcare provider and device manufacturer. The IMDRF (International Medical Device Regulators Forum) suggests ways to standardize rules for personalized medical devices. These suggestions help rules meet across countries and reduce compliance costs. These regulatory pathways aim to balance state-of-the-art technology with patient safety, making sure custom devices are high-quality, safe, and work well.
Conclusion
Titanium 3D printing has altered the map of medical technology and solved many problems with traditional surgical tools and implants. This technology provides unmatched customization capabilities that bridge the gap between standard manufacturing and patient needs. Medical teams can now create patient-specific implants using precise CT/MRI imaging, which eliminates the “one-size-fits-all” approach and leads to better surgical outcomes and patient satisfaction.
Without doubt, titanium’s exceptional biocompatibility, especially with Ti-6Al-4V alloy, makes it perfect for long-term implantation. The material’s natural bone-integration properties, boosted through carefully designed porous structures, help create implants that become part of the patient’s anatomy rather than just foreign objects taking up space.
Complex design and fabrication processes deliver remarkable benefits. Selective Laser Melting technology creates dense, strong components while advanced post-processing techniques ensure these instruments meet strict medical standards. Medical teams use electropolishing and proper sterilization to guarantee reliable performance in clinical settings.
Clinical evidence shows real improvements from this technology. Patient-matched guides substantially reduce operating room time, sometimes cutting procedure length in half. Healthcare facilities and patients both benefit from less anesthesia exposure and faster surgical throughput.
Budget-friendly advantages stand out clearly. Though initial investment costs more, on-demand manufacturing eliminates expensive tooling costs of traditional production methods. Healthcare facilities get production flexibility without compromising quality, which helps especially when creating specialized instruments in small quantities.
Titanium 3D printing keeps expanding into specialized medical fields like foot, ankle, and oncology applications. Teams can achieve even greater precision and efficiency by combining artificial intelligence with advanced surgical planning software. On top of that, regulatory frameworks keep evolving to handle unique challenges of custom medical devices while balancing breakthroughs with safety standards.
This technology represents a transformation in medical device manufacturing—moving from mass production to tailored solutions that fit each patient’s unique anatomy. Modern healthcare’s focus on personalized medicine matches this approach perfectly, which ended up delivering better outcomes and improved quality of life for patients worldwide.
Key Takeaways
Titanium 3D printing is revolutionizing medical device manufacturing by enabling patient-specific solutions that address the limitations of traditional standardized instruments and implants.
• Custom implants from medical imaging: CT/MRI scans enable precise patient-specific titanium implants that match individual anatomy, eliminating the “one-size-fits-all” approach of conventional devices.
• Superior biocompatibility drives better outcomes: Ti-6Al-4V titanium alloy offers exceptional osseointegration properties, allowing implants to form direct structural connections with bone tissue for long-term success.
• Significant OR time reduction: Patient-matched 3D printed surgical guides can reduce procedure times by up to 50%, cutting a 90-minute surgery to 45 minutes while improving placement accuracy.
• Cost-effective on-demand manufacturing: 3D printing eliminates expensive tooling costs (typically $50,000+) and enables production of low-volume specialized instruments without financial risk.
• AI integration enhances surgical precision: Advanced software now automates surgical planning within 20-30 minutes, combining artificial intelligence with 3D printing for optimized implant positioning and surgical outcomes.
This technology represents a fundamental shift toward personalized medicine, where medical devices are tailored to individual patient anatomy rather than forcing patients to adapt to standardized solutions. The combination of titanium’s biocompatibility, 3D printing’s design freedom, and AI-driven planning creates unprecedented opportunities for improved patient care and surgical efficiency.
FAQs
Q1. What are the main advantages of 3D printed titanium surgical instruments? 3D printed titanium surgical instruments offer several key benefits, including customization for specific procedures, improved ergonomics, reduced weight, and the ability to quickly iterate designs based on surgeon feedback. They can also be more cost-effective for low-volume production compared to traditional manufacturing methods.
Q2. How does titanium 3D printing improve patient outcomes in orthopedic surgeries? Titanium 3D printing enables the creation of patient-specific implants that precisely match individual anatomy. This leads to better fit, improved osseointegration, and potentially faster recovery times. Additionally, 3D printed surgical guides can increase the accuracy of implant placement and reduce operating room time.
Q3. What post-processing steps are necessary for 3D printed titanium medical devices? After printing, titanium medical devices typically undergo stress relief and heat treatment to address residual stresses. Surface finishing techniques like electropolishing are then applied to achieve a smooth, defect-free surface. Finally, the devices must be validated for sterilization compatibility, usually through autoclave or gamma irradiation methods.
Q4. How does the cost of 3D printed titanium instruments compare to traditional manufacturing? For low-volume production (typically under 200 units), 3D printing titanium instruments is often more cost-effective than traditional manufacturing. This is primarily due to the elimination of expensive tooling costs, which can exceed $50,000 for conventional methods. 3D printing allows for on-demand production without these upfront investments.
Q5. What future developments are expected in titanium 3D printing for medical applications? The future of titanium 3D printing in medicine is likely to see expansion into more specialized fields like foot and ankle surgery and oncology. Integration with AI and advanced surgical planning software is expected to further enhance precision and efficiency. Additionally, regulatory frameworks are evolving to address the unique challenges of custom 3D-printed medical devices.

